What are Nervous System Diseases?
Types of Nervous System Diseases
- Stroke
- Coma
- Neurological disorders such as (ALS, Parkinson’s Disease, Alzheimer’s disease and other dementias)
- Neurological malignancies
Stroke
A stroke occurs when a blood clot or a break in a vessel in the brain causes an interruption of blood flow to an area of the brain. Symptomology depends on the amount of damage that occurred and the area of the brain that was affected by the stroke.
Coma
Coma is a deep state of unconsciousness. It can be caused by disease, injury, or poison.
What is the Prognosis?
Individuals with nervous system diseases may die from:
- sepsis.
- lack of food and fluids as a result of a decision not to insert a feeding tube in a patient that cannot swallow.
- lack of oxygenation as a result of a decision not to initiate mechanical ventilation.
- lack of the ability to maintain a heartbeat or breathe on one’s own due to withdrawal of life support.
Palliative Care
Pharmacological and non-pharmacological interventions should focus on symptomatic relief, prevention of complications, maintenance of maximum function and optimal quality of life.
Psychological and spiritual support is needed to assist caregivers who may be providing full care around the clock care for their loved one. Provide caregivers with resources, respite care and support groups in their area.

CONTINUA LEARNING
Simplify Your Hospice Team’s Training and Skill Building
A complete solution for your agency: more than 125 hospice courses, caregiver in-services, training plans, and more.
Documentation
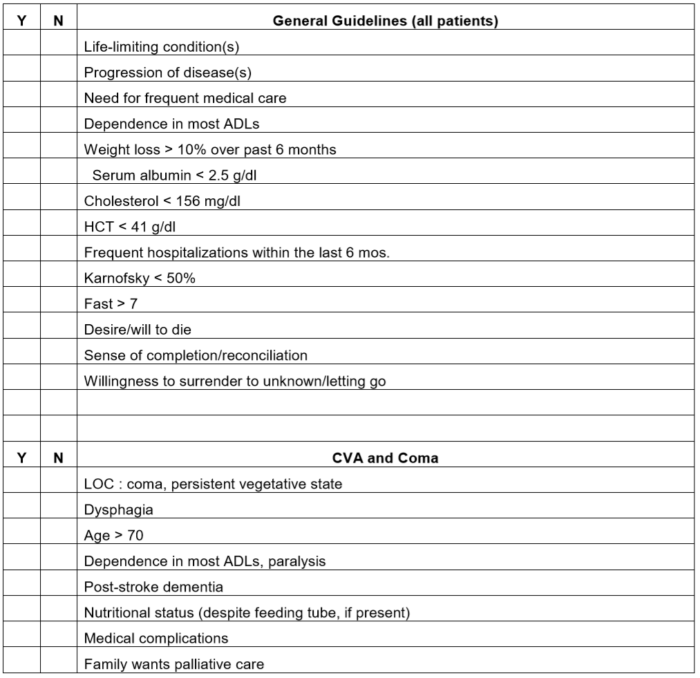
During the acute phase immediately following a hemorrhagic or ischemic stroke, any of the following are strong predictors of early mortality and should be documented:
- Coma or persistent vegetative state secondary to stroke, beyond three days duration
- Coma or severe obtundation accompanied by severe myoclonus, persisting beyond three days past the anoxic event
- Comatose patients with any 3 of the following symptoms on day three of coma (97% mortality by two months)
✓ abnormal brain stem response
✓ absent verbal response
✓ absent withdrawal response to pain
✓ serum creatinine > 1.5 mg/dl
✓ age > 70
✓ dysphagia — document if severe enough to prevent food and fluid intake necessary to sustain life
During the chronic phase, document the following factors which may correlate with poor survival following severe stroke:
- age > 70
- poor functional status, Karnofsky Performance Scale score < 50%
- post-stroke dementia, Functional Assessment Status Tool score > 7
- aspiration pneumonia without effective response to speech therapy interventions
- poor nutritional status, whether on artificial nutrition or not on artificial nutrition
- unintentional progressive weight loss of greater than 10% over past 6 months
- serum albumin less than 2.5 gm/dl (a useful indicator but should not be used alone)
References
Fallon, M. Palliative Medicine in non-malignant disease. In: Doyle D, Hanks G, Cherny N, Calman, K. (eds.) (2005). Oxford Textbook Palliative Medicine. 3rd ed. Pp. 844 – 845, Oxford University.
Grauer P, Shuster J & McCrate-Protus B. (2008). Palliative Care Consultant: A reference guide for palliative care 3RD Kendall/Hunt publishing Co. ed.
Kuebler KK, Davis MP & Moore CD. (2005). Palliative Practices: An Interdisciplinary Approach. Elsevier/Mosby: Missouri.
Kinzbrunner B. Non-malignant terminal diseases: criteria for hospice admission. Hosp Update 3: 3- 6, 1993.
Stuart B, et al. Medical Guidelines for Determining Prognosis in Selected Non-Cancer Diseases. Arlington, VA, National Hospice Organization, 1996.
If you found this article informative and useful share it with your friends and colleagues.
